

Repetitive transcranial magnetic stimulation (rTMS) has taken the world of neurological rehabilitation by storm the last few decades, offering a safe, effective, non-invasive treatment for a range of neurologic and psychiatric conditions. rTMS is proven to be particularly effective when used in conjunction with other neurorehabilitation therapies and treatments.
HOW DOES IT WORK?
rTMS utilizes electromagnetic pulses to directly stimulate areas of the brain that have been damaged or are not fully functioning. We know that neurons, or brain cells, use electrical charges to communicate with one another. However, after a brain injury or with psychiatric disorders, these neurons struggle to fire correctly due to an electrical imbalance.
By sending a rapid series of painless electromagnetic pulses into these neurons, the rTMS can effectively reset the electrical charge of the neurons so that they can fire appropriately. This improved function is sustained long after receiving the treatment, as the neurons have essentially been given a gentle jumpstart that shifts them back into harmony.
THE HISTORY OF rTMS
The history of rTMS actually dates back to discoveries made in the 1800s, when scientists first learned that neurons, or brain cells, carry an electrical charge. With further discoveries in the 1800s around using magnetic waves to generate electrical charges, it became clear that magnetism would have a significant role to play in neurologic and psychiatric conditions.
The first rTMS device was invented in 1985 and was initially utilized to positively affect and upregulate the frontal lobe of depression and PTSD patients with a high degree of success. Researchers and clinicians quickly realized that the benefits of rTMS could likely reach a much larger audience, particularly in the arena of traumatic brain injury (TBI), concussion, and stroke recovery, so the research began to expand rapidly.
Initial studies showed very promising results for brain injury patients, particularly in the area of neuroprotection and recovery after a TBI. Over the course of the last 35 years, the data has continued to pour in from all over the world, adding to the excitement surrounding the potential for rTMS as a cornerstone of neurologic and psychiatric care. rTMS is FDA-approved for a range of conditions, and that list continues to grow as the research discovers more uses for this therapy, such as rehabilitating the motor areas, speech areas, and more.
WHEN IS rTMS USED?
rTMS is used for many of our patients at Resiliency, though it must first be deemed appropriate by the doctor who performs the examinations and evaluations. Since every patient and every brain is unique, this is decided on a case-by-case basis.
We are using it to help many of our TBI and concussion patients suffering from symptoms of insomnia, chronic pain, memory loss, anxiety, stroke, and many more due to its widespread applications.
HOW IS rTMS ADMINISTERED?
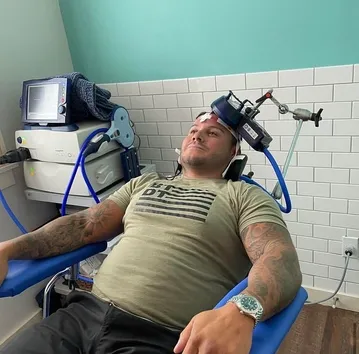
Once rTMS has been prescribed to a patient, the patient sits in a chair that we recline back according to the patient’s preferences for maximum comfort. One of our doctors will then place a locator cap over the patient’s head, which essentially maps out the regions of the brain and ensures that the pulses are delivered in the precise targeted area.
Using this cap, the doctor will bring the rTMS magnet to the patient’s head, so it is gently touching the precise area that needs to be stimulated. Next, the doctor will begin the treatment, which sends a series of pulses through the scalp and skull, into the targeted area of the brain.
This lasts for about 7 minutes, since it is rapid TMS, remarkably condensing a traditionally lengthy treatment into a short, relaxing experience. It is recommended to allow the body and mind to relax by breathing slowly and settling into a meditative state while receiving the therapy.
After the treatment has been completed, the doctor will assist the patient in removing the cap and getting out of the chair.
To find out if you would benefit from rTMS, please fill out this contact form.
Research: